Results from the Migraine in Aotearoa New Zealand Survey 2022
Migraine disease is not a loner. It has lots of friends among other long-term health conditions that it likes to hang out with. People with migraine disease are more likely to be affected by anxiety, depression, irritable bowel syndrome, insomnia, fibromyalgia, endometriosis, epilepsy, arthritis, stroke and even asthma, although the risk varies. And that’s not a comprehensive list.
Some of these are fellow neurological conditions, like epilepsy and stroke. Others can be related to brain chemistry, like anxiety, depression and irritable bowel syndrome. The gut contains 90% of the body’s serotonin, which is a hormone that acts on the brain and throughout the body, so this connection to the bowel might not be as strange as it appears. Many conditions that involve chronic pain, like irritable bowel syndrome, endometriosis and fibromyalgia, may have similar impacts on the brain, causing pain receptors to become overly sensitive.
Some conditions have no obvious relation to the brain, like asthma, rheumatoid arthritis and heart disease, but a common link might be inflammation. Understanding more about why these other health conditions are associated with migraine could help with developing treatments that target a shared cause.
In the Migraine in Aotearoa New Zealand Survey 2022, we asked respondents whether they had any other long-term health conditions. Most people had another condition, with only 22% reporting that they currently had none.
The most common conditions were mood disorders, with almost a third (32%) reporting anxiety and almost a quarter (24%) reporting depression. Around one in five reported low back pain (21%) and irritable bowel syndrome (18%). Asthma occurred in 16% of respondents, insomnia in 13% and high blood pressure in 11%. Less than 10% reported arthritis (8%) and fibromyalgia (6%). Heart disease and stroke were uncommon (<1%).
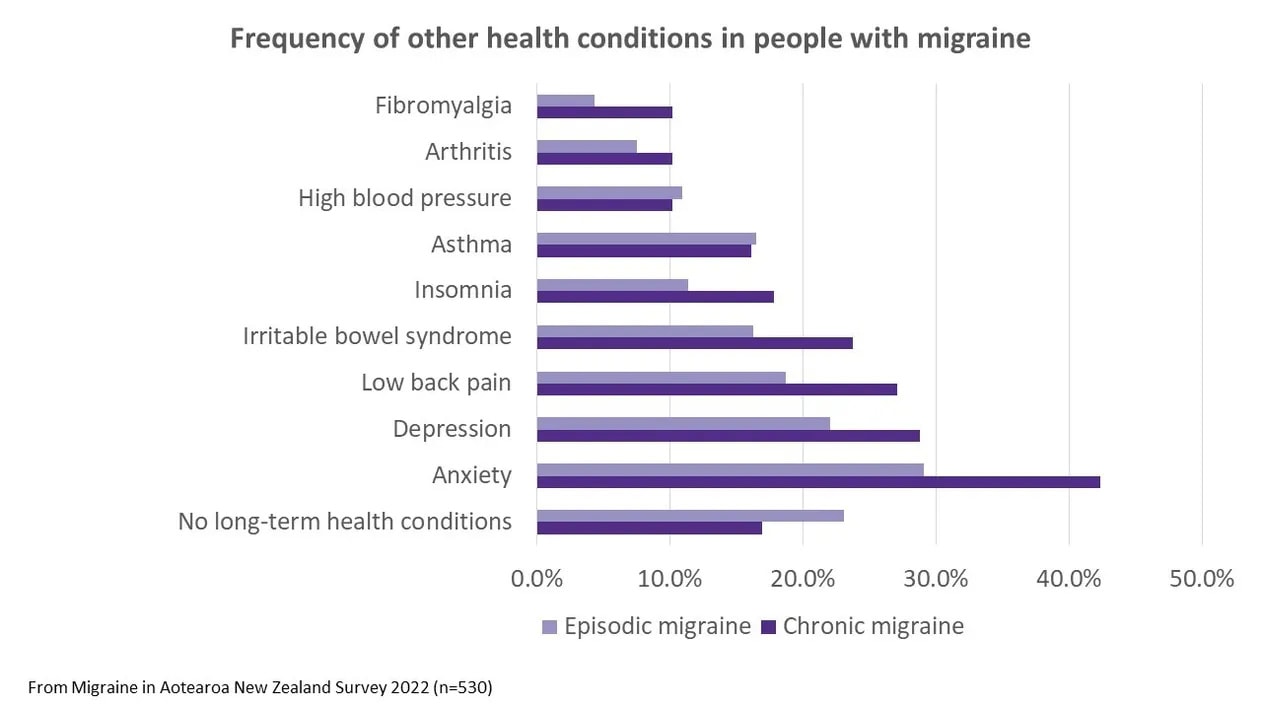
Some of these conditions were more commonly reported in people with chronic migraine than those with episodic migraine*. Mood disorders, pain and insomnia can be involved in driving recurrent migraine attacks, in an intertwined cycle. For example, disrupted sleep may be a trigger for an attack, and migraine pain can interfere with sleep, but sleep can also be restorative and help end an attack.¹
Survey respondents also reported conditions we didn’t specifically ask about, so these will underestimate how frequently they actually occur in people with migraine. Overall, around 3% of people had a fatigue-related condition (chronic fatigue syndrome/myalgic encephalopathy or long COVID), endometriosis or another mental health condition (not anxiety or depression). Another 2% had diabetes, thyroid disease or another pain condition. Celiacs disease, Ehlers Danlos and postural orthostatic tachycardia syndrome (POTS) were reported by 1% or fewer.
One of the reasons it’s important to consider other health conditions in someone with migraine is that this can help with treatment choices. Someone with frequent migraine attacks and depression might do well-taking amitriptyline or nortriptyline, which are also antidepressants. Someone with insomnia may also be helped with amitriptyline (which is sedating). If you have asthma, you shouldn’t take beta blockers.
It’s also important to ensure that other health conditions are well managed, as this can improve migraine symptoms. Studies have found that treatment for anxiety can reduce the number of migraine attacks,² and so can treatment for insomnia,³ independent of any migraine intervention. Conversely, treatment of migraine might also help manage other conditions – treatment with migraine-specific medication (calcitonin gene-related peptide monoclonal antibodies) can reduce symptoms of anxiety and depression.⁴
However, this too can be complicated. In a study of Emgality (galcanezumab), people with chronic migraine and anxiety or depression only experienced a significant reduction in headache days with 240mg of the drug,⁵ which is double the dose we use in NZ (and would be double the price if we wanted to try it).
As usual, more research is needed to find and target the causes for why migraine travels with all these other ailments. It might help to know that having other health conditions as well as migraine isn’t a sign you’re broken or weak or hypochondriac. There are reasons for these associations that are outside our control, biological processes in the body that make the coexistence of all these conditions much more likely. We don’t yet understand all the connections, but ongoing research continues to improve our understanding, and maybe someday, we will.
References
- Proserpio, P. & Agostoni, E. C. The spectrum of migraine comorbidities: Sleep and migraine. Neurological Sciences 41, S437–S438 (2020).
- Karimi, L., Wijeratne, T., Gillard Crewther, S., Evans, A. E. & Ebaid, D. The Migraine-Anxiety Comorbidity Among Migraineurs: A Systematic Review. Frontiers in Neurology 11, 613372 (2021).
- Walker, D., Zhang, N. & Natbony, L. R. Insomnia and Migraine: A Review of Evidence-Based, Biobehavioral Interventions. Curr Pain Headache Rep (2023) doi:10.1007/S11916-023-01100-X.
- Rhyne C, Cohen JM, Seminerio MJ, Carr K, Krasenbaum LJ. Burden of migraine with acute medication overuse or psychiatric comorbidities and treatment with CGRP pathway-targeted monoclonal antibodies: A review. Medicine (Baltimore). 2023 Jun 9;102(23):e33874
- Smitherman, T. A. et al. Efficacy of Galcanezumab for Migraine Prevention in Patients With a Medical History of Anxiety and/or Depression: A Post Hoc Analysis of the Phase 3, Randomized, Double-Blind, Placebo-Controlled REGAIN, and Pooled EVOLVE-1 and EVOLVE-2 Studies. Headache: The Journal of Head and Face Pain 60, 2202–2219 (2020).


